Migraine Headache
Irritated Pituitary Gland
Migraine headaches affect more than 30 million Americans – including 10% of children. A migraine is a severe, debilitating form of headache that typically appears as a throbbing ache near the side of the forehead. Migraines are considered a type of vascular headache because, in addition to nerves and chemicals, they involve the blood vessels in the brain. Migraines are most likely caused by an abnormal trigger of chemicals that cause these blood vessels to swell. But, which chemicals are responsible? Why do these chemicals bother some people but not others? And most importantly, how can they be overcome, thereby eliminating the migraine?
Genetic Links to Migraines
According to the National Headache Foundation (NHF), 70 to 80 percent of migraine sufferers have a family history of migraines. Many foods have been linked to migraines, including chocolate, red wine, cheeses, processed meats and foods with the preservative MSG. Caffeine and alcohol have also been implicated. What is interesting about these foods is that each one of them has a special detoxification pathway in the liver; a pathway that can easily be disrupted by nutritional deficiencies and genetic issues. For instance, craving chocolate is often linked to a zinc or magnesium deficiency. These two minerals are the most important in the body for proper DNA replication via enzyme activation. If enzymes do not perform as designed, the results are mutated DNA strands and the eventual expression of “bad” genes. Cheeses often contain molds. Mold toxins are called mycotoxins and have a direct link to poor DNA replication as well as being a significant stress on the liver. Processed meats contain sulphites as do wines. A high percentage of people do not possess adequate nutrients to aid in the detoxification of sulphites. Molybdenum, a trace mineral needed in only small amounts, can often help this particular detoxification pathway. And finally, around 10 percent of people genetically do not adequately breakdown glutamate (as in Monosodium glutamate (MSG)) into glutamine. Again we see another genetic/enzyme link to migraines. But how did these bad genes get expressed? Or, how did the migraine sufferer get these headaches in the first place? Here are some clues:
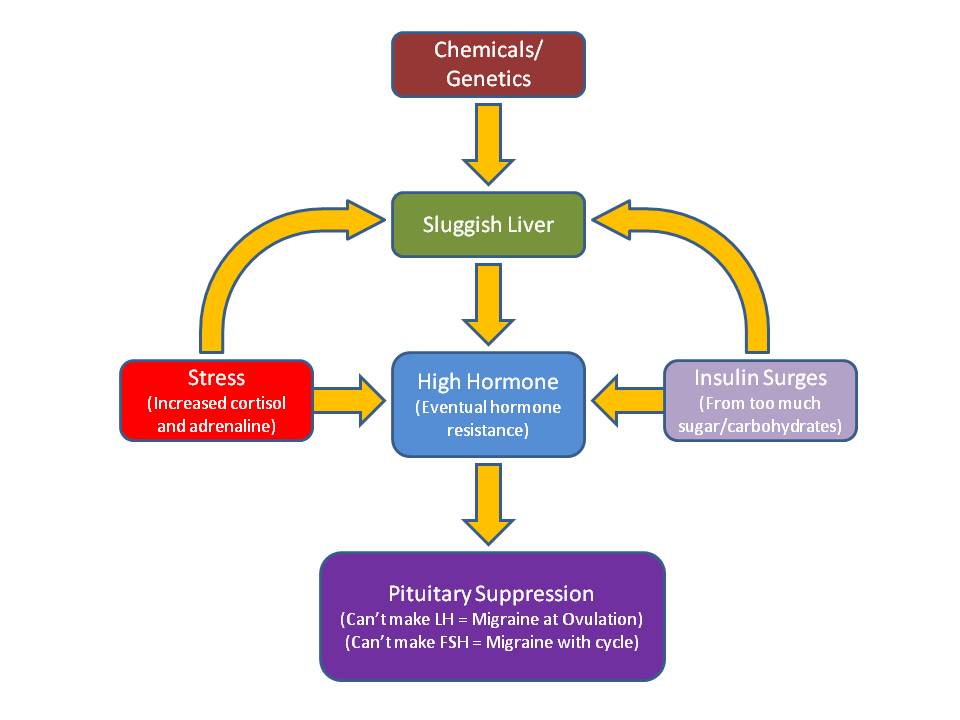
From the above facts it should be easy to recognize that there is a hormonal trigger with most migraines. However, the hormones need not only be related to the reproductive system. Stress, which induces high levels of cortisol and adrenaline, can also trigger migraines. Also, insulin, when released as a result of blood sugar swings, is culpable. So what is the link to all of these different hormones? - The pituitary gland.
All of the migraine cases that I have helped successfully eliminate (yes, you can eliminate migraines in most people), no matter which other chemicals were found, there was always a strong connection to the pituitary gland.
The Pituitary
The pituitary gland is located about one to two inches directly behind the bridge of your nose. It is the gland in the body once referred to as the master gland. This name was appropriate because no hormones are secreted in the body unless first told to do so by other hormones from the pituitary gland. For instance, if extra thyroid hormones are needed, the pituitary will send out a hormone called thyroid stimulating hormone (TSH). If extra adrenal hormones are required to fight stress, the pituitary will send out a hormone called ACTH. If a woman’s progesterone is low, the pituitary sends out luteinizing hormone (LH). If low estrogen is the issue, then out goes follicle stimulating hormone (FSH), etc. This response by the pituitary is based on a negative feedback loop. In other words, when a hormone begins to get low, the pituitary must become activated or facilitated so as to increase the low hormone. When a hormone becomes high, the pituitary must become inactivated or inhibited so that the hormone does not become too high (it is the liver’s job to eliminate excess hormone).
So, what happens if this very important gland does not properly perform its vital functions because it is either over or under stimulated? Since hormones control just about everything, then just about anything symptomatically can potentially occur. The most common problem I see with the pituitary gland is low function or suppression. That is, the pituitary just simply does not respond even when it is supposed to. Therefore, if estrogen drops, a suppressed pituitary gland does not respond with FSH and the net result is continued low estrogen. But here is the tricky part. When the pituitary is functionally suppressed, further suppression equals significant symptoms to the body as a whole. The three most likely pituitary suppressants in my testing are: insulin, white sugar and cortisol. So once again we see that when under stress (cortisol increase) sweets are craved and ingested (sugar) resulting sooner or later in hypoglycemia (insulin surges) or insulin resistance, all of which further suppress the pituitary and dysregulate the hormonal system. There is however another important reason why the pituitary becomes suppressed – too much hormone. Remember that the pituitary, through negative feedback, becomes inhibited by too much hormone. This should rarely happen if the detoxification pathways in the liver are adequate. All too often this is not the case. A sluggish liver will result in high hormonal levels in the body. Eventually, as a protective mechanism by the body, cells will become resistant to the high hormonal levels, because too much hormone is worse than not enough. This phenomenon of hormonal resistance is the reason why a woman who has plenty of estrogen will act as though she has very little (hot flashes, vaginal dryness). If she takes estrogen, she feels terrible. I will discuss these phenomena further in an upcoming newsletter. For now, take
Genetic Links to Migraines
According to the National Headache Foundation (NHF), 70 to 80 percent of migraine sufferers have a family history of migraines. Many foods have been linked to migraines, including chocolate, red wine, cheeses, processed meats and foods with the preservative MSG. Caffeine and alcohol have also been implicated. What is interesting about these foods is that each one of them has a special detoxification pathway in the liver; a pathway that can easily be disrupted by nutritional deficiencies and genetic issues. For instance, craving chocolate is often linked to a zinc or magnesium deficiency. These two minerals are the most important in the body for proper DNA replication via enzyme activation. If enzymes do not perform as designed, the results are mutated DNA strands and the eventual expression of “bad” genes. Cheeses often contain molds. Mold toxins are called mycotoxins and have a direct link to poor DNA replication as well as being a significant stress on the liver. Processed meats contain sulphites as do wines. A high percentage of people do not possess adequate nutrients to aid in the detoxification of sulphites. Molybdenum, a trace mineral needed in only small amounts, can often help this particular detoxification pathway. And finally, around 10 percent of people genetically do not adequately breakdown glutamate (as in Monosodium glutamate (MSG)) into glutamine. Again we see another genetic/enzyme link to migraines. But how did these bad genes get expressed? Or, how did the migraine sufferer get these headaches in the first place? Here are some clues:
- Women have migraines three times more often than men, according to the NHF.
- 75% of women get migraines at ovulation or near the start of their cycle.
- Migraines occur most often between ages 15 and 55. [the time when most women are menstruating]
- Common triggers of migraines include noise, light, hormonal changes, sleep disturbances, stress and intensive physical activity.
From the above facts it should be easy to recognize that there is a hormonal trigger with most migraines. However, the hormones need not only be related to the reproductive system. Stress, which induces high levels of cortisol and adrenaline, can also trigger migraines. Also, insulin, when released as a result of blood sugar swings, is culpable. So what is the link to all of these different hormones? - The pituitary gland.
All of the migraine cases that I have helped successfully eliminate (yes, you can eliminate migraines in most people), no matter which other chemicals were found, there was always a strong connection to the pituitary gland.
The Pituitary
The pituitary gland is located about one to two inches directly behind the bridge of your nose. It is the gland in the body once referred to as the master gland. This name was appropriate because no hormones are secreted in the body unless first told to do so by other hormones from the pituitary gland. For instance, if extra thyroid hormones are needed, the pituitary will send out a hormone called thyroid stimulating hormone (TSH). If extra adrenal hormones are required to fight stress, the pituitary will send out a hormone called ACTH. If a woman’s progesterone is low, the pituitary sends out luteinizing hormone (LH). If low estrogen is the issue, then out goes follicle stimulating hormone (FSH), etc. This response by the pituitary is based on a negative feedback loop. In other words, when a hormone begins to get low, the pituitary must become activated or facilitated so as to increase the low hormone. When a hormone becomes high, the pituitary must become inactivated or inhibited so that the hormone does not become too high (it is the liver’s job to eliminate excess hormone).
So, what happens if this very important gland does not properly perform its vital functions because it is either over or under stimulated? Since hormones control just about everything, then just about anything symptomatically can potentially occur. The most common problem I see with the pituitary gland is low function or suppression. That is, the pituitary just simply does not respond even when it is supposed to. Therefore, if estrogen drops, a suppressed pituitary gland does not respond with FSH and the net result is continued low estrogen. But here is the tricky part. When the pituitary is functionally suppressed, further suppression equals significant symptoms to the body as a whole. The three most likely pituitary suppressants in my testing are: insulin, white sugar and cortisol. So once again we see that when under stress (cortisol increase) sweets are craved and ingested (sugar) resulting sooner or later in hypoglycemia (insulin surges) or insulin resistance, all of which further suppress the pituitary and dysregulate the hormonal system. There is however another important reason why the pituitary becomes suppressed – too much hormone. Remember that the pituitary, through negative feedback, becomes inhibited by too much hormone. This should rarely happen if the detoxification pathways in the liver are adequate. All too often this is not the case. A sluggish liver will result in high hormonal levels in the body. Eventually, as a protective mechanism by the body, cells will become resistant to the high hormonal levels, because too much hormone is worse than not enough. This phenomenon of hormonal resistance is the reason why a woman who has plenty of estrogen will act as though she has very little (hot flashes, vaginal dryness). If she takes estrogen, she feels terrible. I will discuss these phenomena further in an upcoming newsletter. For now, take
Fixing the problem
To correct a migraine pattern, each of the disrupted areas above must be fixed as much as possible. This is not as hard as it sounds. Chemicals are detoxified; genetics are often overcome with proper enzyme co-factors like zinc and magnesium; stress can be reduced with PAK and emotional balancing; the chemicals of stress modulated; insulin can be managed with a hypoglycemic diet and proper nutrients; and the pituitary itself can be awoken with the correct herbal support (Chaste tree and maca root are often helpful). Correcting migraines with this approach is very often achievable.
To correct a migraine pattern, each of the disrupted areas above must be fixed as much as possible. This is not as hard as it sounds. Chemicals are detoxified; genetics are often overcome with proper enzyme co-factors like zinc and magnesium; stress can be reduced with PAK and emotional balancing; the chemicals of stress modulated; insulin can be managed with a hypoglycemic diet and proper nutrients; and the pituitary itself can be awoken with the correct herbal support (Chaste tree and maca root are often helpful). Correcting migraines with this approach is very often achievable.